This post, as titled, is a follow-up to last week’s:
The "cytokine storm is not real" study
The study has now been online for a few weeks, and may already be familiar to the reader: The text is dense and confusing — it is not immediately clear how the authors reach many of their conclusions — so this review was delayed. Claimed study findings:
Which regards the following study:
i. Who was in the study? Could “cytokine storm” have been missed?
Gao, et al. provide a graphical overview of the study design, and due to basing my post on the same, I described the design inaccurately as including 585 patients who had ICU stays for “severe pneumonia,” 190 of which were related to infection with SARS-CoV-2.
However, the methods section reveals that the study only includes patients in the ICU who underwent a Bronchoalveolar Lavage with screening for bacterial infection. Hat-tip to Modern Discontent for pointing out the correct reading in the comments, as well as in his own review of the study which is more thorough than my own:
In this respect, it would have been better to focus on the term “respiratory failure” in the graphical description, as this describes ICU care directed on respiratory support, the most common reason for ICU care even before this virus.
Does this imply that some number of real-life patients have severe disease and death under different conditions than measured by this study?
In one of the earliest large samples of outcomes for patients hospitalized for “Covid-19,” from spring of 2020 in New York City, roughly half (271) of 553 deaths occur without mechanical ventilation.1 In a more recent study covering outcomes from all of 2020, among patients receiving any type of respiratory assistance (including non-invasive) in an ICU setting, half of whom are not initially mechanically ventilated, 27% of all deaths (209 of 769) occur without patients preceding to ventilation beforehand.2
If these ratios were maintained for the hospitals sampled by Gao, et al., it would further disqualify the paper from making any strong case that “secondary pneumonia” from bacterial infections drive most deaths; but would also limit conclusions ruling out (the myth of) cytokine storm completely. Likely half or more deaths among those hospitalized for “Covid-19” involve ventilation beforehand (the “or more” includes an assumption that ventilator use increased after 2020), what if the rest are “cytokine storm”?
Of course, any such conclusions would require contradicting the studies that already addressed this topic directly, as reviewed in Tolerance and Severe Disease Pt. 1; these direct investigations are more important than Gao, et al. because they actually measure cytokines and capture the state of patients before ICU admission. Specifically, Remy, et al. report that:
Circulating cytokines in COVID-19 patients, at least early in their clinical course, did not show widespread elevation. Most COVID-19 patients had either no elevation or only mild increases in the major proinflammatory cytokines including TNF-α, IL-1α, IL-1β, IFN-ɣ, etc3
ii. High-ish cytokines are not “cytokine storm”
As for what kills patients who do not make it to the ventilator for respiratory failure, there is certainly a role here for inflammation in contributing to coagulation cascades and thrombosis. However, attributing clotting pathologies to inflammation directly renders matters over-determined. The SARS-CoV-2 spike protein contributes to clotting even in absence of platelets (as shown by Pretorius et al.4); that it is also pro-inflammatory exacerbates clotting (as shown by Pretorius et al.5) but does not exclusively cause it. Spike disrupts endothelial junctions,6 other viral proteins possibly trigger vascular mitochondria dysfunction and cell death and sabotage hypoxic vasoconstriction7 — and all of these can contribute to cardiac and brain harms and death by essentially strangling these vital organs until they give up, even in advance of formally diagnosed respiratory failure. Medications for the virus, namely nucleoside analogs like Remdesivir and Molnupiravir, might contribute to kidney or cardiac failure as well. So there are plenty ways besides respiratory failure that the virus (and treatment for it) can kill, yes.
None of this requires or is proof of “cytokine storm” — this would require any evidence, anywhere, that such “storms” are actually occurring in terms of extremely high levels of circulating cytokines, and the evidence does not exist, because the phenomenon does not occur in severe Covid-19 (which, again, is more characterized by immune suppression).
However, several comments in reply to last week’s post simply endeavored to defend “cytokine storm” by pointing out that cytokines are elevated at all, in infection and severe disease. But cytokines are meant to be elevated in any infection; and levels observed for SARS-CoV-2 are not any higher than normal in this context, similar to flu (again, as reviewed in TASD pt. 1).
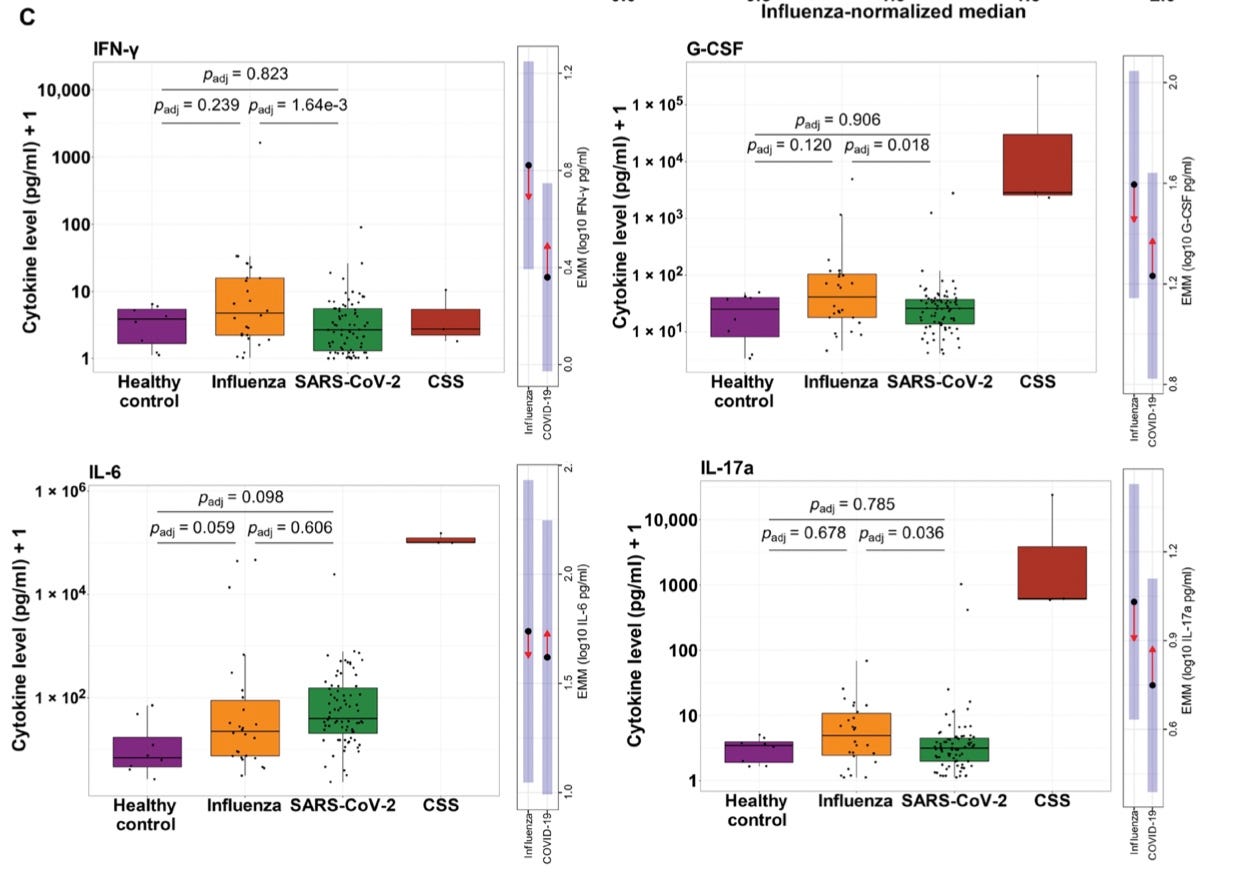
Nor can long-term (as in post-acute) elevations of inflammatory markers act as a proxy for the non-existent, missing evidence of any acute explosion of the same. It simply isn’t a thing, and the only “evidence” otherwise, again, are the assumptions made in advance of any evidence back in 2020.
iii. Piercing the myth
My review of Gao, et al. should have stated more clearly that the study is not an overwhelming refutation of the “cytokine storm” myth in of itself. However, it does not need to be any such thing; the evidence has already been compelling since 2020 that cytokine storm is not a real factor of severe Covid-19.
What is more remarkable, is that the study has generated headlines finally poking in the direction of the balloon that is the myth.8 It is for this reason that the title of last week’s post included quotation-marks in the title — what is notable about the study is that it is leading to people saying cytokine storm is not real (which is true), whereas for three years all people have been saying, absent a shred of evidence, is that it is real (which is false).
With these statements being made, the onus (hopefully) is finally on those who (even to this day) wish to keep recycling the myth in publications regarding SARS-CoV-2 to “show their work” on the claim that an “out-of-control” immune response is the cause of severe disease in SARS-CoV-2 infections — which said myth-recyclers will not be able to do. And so the myth (hopefully) must finally be dispelled, allowing a clearer view of what the virus was, and how it killed (by… infecting people).
If you derived value from this post, please drop a few coins in your fact-barista’s tip jar.
https://jamanetwork.com/journals/jama/fullarticle/2765184 - will add formatting to footnotes later, currently on mobile
https://www.medrxiv.org/content/10.1101/2022.12.19.22283704v1
Remy, KE. et al. “Severe immunosuppression and not a cytokine storm characterizes COVID-19 infections.” JCI Insight. 2020 Sep 3; 5(17): e140329.
Reviewed in TASD pt. 1:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8380922/
https://www.biorxiv.org/content/10.1101/2021.10.12.464152v1.full
https://www.frontiersin.org/articles/10.3389/fcvm.2021.687783/full
Archer, SL. et al. “SARS-CoV-2 mitochondriopathy in COVID-19 pneumonia exacerbates hypoxemia.” Redox Biology, online ahead of press at sciencedirect.com.
Reviewed in “The SARS-CoV-2 and Blood Going to Air-less Lung Areas Study”
While also, sadly, generating headlines around a new myth of secondary infections driving “most” deaths.












Maybe part of the reason for the continued existence of the cytokine-storm story is that immune suppression treatment (like corticosteroids? Prednisone?) seemed to work.
Makes sense. That is why I could never be successful as a research scientist. I don’t play well with liars and cowards.